Written by Jeff Roberts
A team of Australian researchers are using a non-invasive ultrasound technology to assist in removing toxic plaque and lesions from nerve cells commonly associated with the onset of Alzheimer’s disease.
If you are one of the many millions of people who have witnessed the degenerative effects of Alzheimer’s disease, then you likely know how heartbreaking it is to see a loved one’s quality of life dissipate in what seems like an instant.
For years, scientists have worked diligently to find a counteractive treatment for the common neuro-degenerative disease, but mostly with no successful avail. Thankfully, however, this might all be about to change.
A team of researchers from the Queensland Brain Institute (QBI) at the University of Queensland have found success in reversing the processes that are commonly associated with the onset of Alzheimer’s and other dementia-related diseases. Their findings were published in the journal Science Translational Medicine.
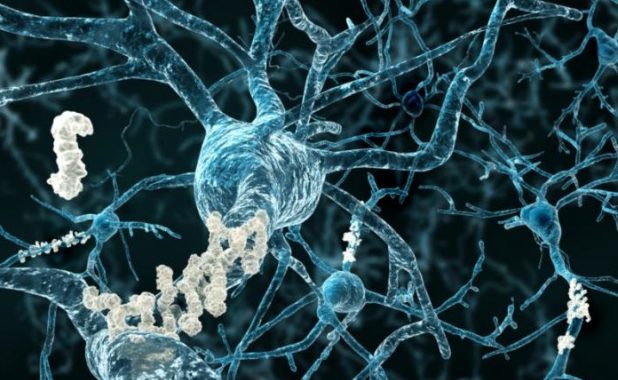
From what we currently understand, a person’s Alzheimer’s disease is usually the result of a build-up of two types of lesions – amyloid plaques, and neurofibrillary tangles. Amyloid plaques sit between the neurons and end up as dense clusters of beta-amyloid molecules, a sticky type of protein that clumps together and forms plaques.
Neurofibrillary tangles are found inside the neurons of the brain, and they’re caused by defective tau proteins that clump up into a thick, insoluble mass. This causes tiny filaments called microtubules to get all twisted, which disrupts the transportation of essential materials such as nutrients and organelles along them, sort of like when you twist up the vacuum cleaner tube.
The team’s technique uses a particular type of ultrasound called a focused therapeutic ultrasound, which non-invasively beams sound waves into the brain tissue. By oscillating super-fast, these sound waves are able to gently open up the blood-brain barrier, which is a layer that protects the brain against bacteria, and stimulate the brain’s microglial cells to activate.
Microglila cells are basically waste-removal cells, so they’re able to clear out the toxic beta-amyloid clumps that are responsible for the most severe symptoms of Alzheimer’s.
Remarkably, the team reports a 75% success rate in fully restoring memory function for the rats they tested the treatment on. Even better is the fact that there was no brain damage to surrounding tissues.
They found that the treated mice displayed improved performance in three memory tasks – a maze, a test to get them to recognize new objects, and one to get them to remember the places they should avoid.
“We’re extremely excited by this innovation of treating Alzheimer’s without using drug therapeutics,” one of the team, Jürgen Götz, said in a press release. “The word ‘breakthrough’ is often misused, but in this case I think this really does fundamentally change our understanding of how to treat this disease, and I foresee a great future for this approach.”
The team says they’re planning on starting trials with higher animal models, such as sheep, and hope to get their human trials underway in 2017.

Untreated Alzheimer’s mouse (left) and treated with ultrasound (right)
This type of success rate could spell big things for Alzheimer’s treatment. What implications would this have for people suffering from the disease? Could this potentially lead to increased life spans and extended brain capacity and function for the elderly population? These questions and more will continue to be explored with further research, stay tuned for more updates as they come.
What are your thoughts on this news? Share with us in the comment section below!
Source:
http://stm.sciencemag.org/content/7/278/278ra33
http://www.futuretimeline.net/blog/2015/03/14-2.htm#.VTWP6Dt4qd3
Originally posted @ Collective Evolution